Eczema
While there are multiple forms of eczema, the most common form is atopic eczema (also known as atopic dermatitis). The condition is a very common one, often presenting in early childhood - but it can also appear, or recur later in life. Typically, eczema is considered to be a long-term issue, which means it’s a chronic condition.
Overview
Eczema generally presents as itchy, dry or cracked skin that’s often very sore. The condition may be worsened by environment, illness or stress, and patients with eczema may experience periods called ‘flare ups,’ brought on by these factors. Some people also find that their eczema may ‘go dormant’ during some periods of the year, and is influenced by seasonal changes, or temperature.
As a result of the chronic, painful and sometimes unpredictable nature of the condition, many patients find that it negatively impacts their quality of life and self-confidence – particularly as the stress of experiencing and managing eczema can trigger the onset of, or prolong the duration of, an outbreak. Eczema affects one in five children, and often develops before their first birthday, however it is possible to develop eczema at any age, for a variety of reasons.
The condition is seen as likely to be influenced by genetics, so it is possible that if an individual’s parents have experienced problems with eczema, they may be more likely to have the same trouble. Dermatologists have also observed that patients with asthma, hay fever and other allergies can be more prone to developing the condition. All of these conditions are known collectively as the atopic conditions.
While eczema can be a painful and frustrating condition, it is possible that mild or infrequent outbreaks can resolve or ameliorate without further intervention, if careful attention is taken to reduce triggering factors and the use of regular moisturisers. However, patients who experience more frequent or severe outbreaks are likely to require medical attention. In such cases, specialist dermatological intervention is recommended to provide relief and to manage eczema.
Symptoms of Eczema
Acne can appear anywhere on the body – except the palms of the hands and soles of the feet, which do not have sebaceous glands - but the condition most commonly presents on the face, back, chest, shoulders or arms.
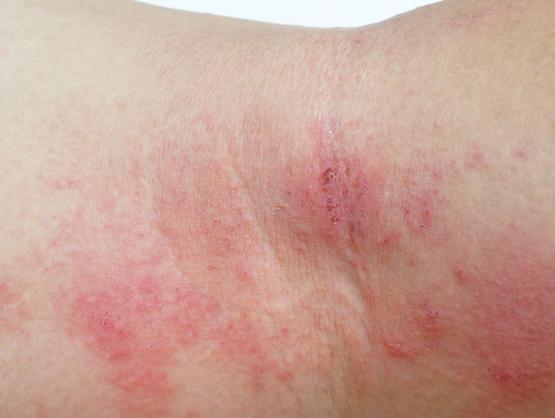
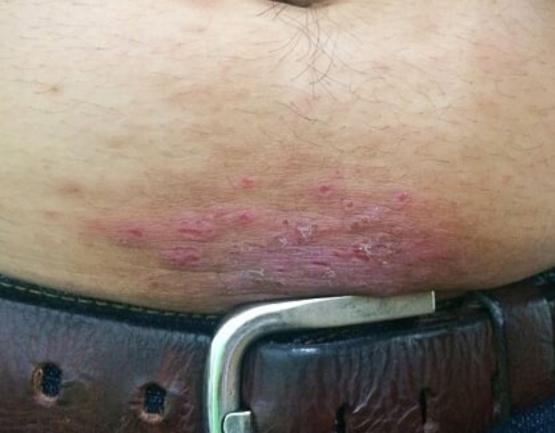
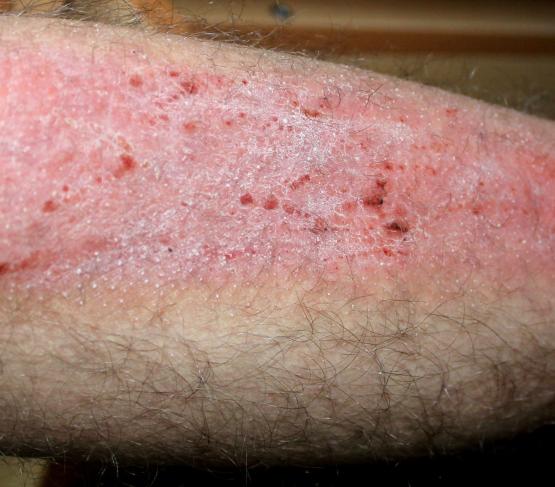
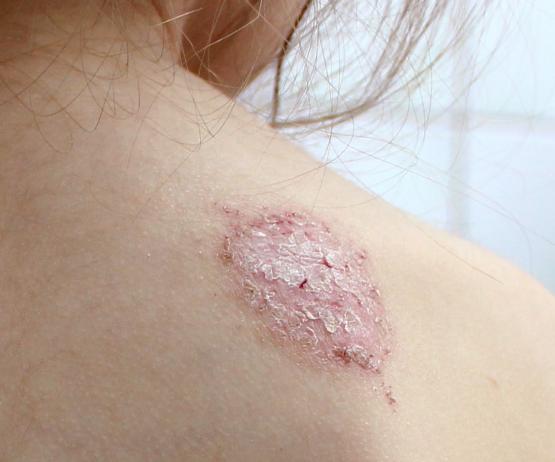
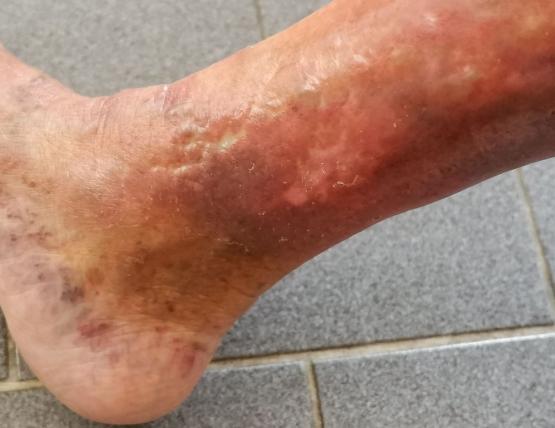
The symptoms of eczema are itchy, dry and cracked skin that can become very uncomfortable, and often sore. It can present anywhere on the body, but often appears on the hands, cheeks, chin, chest, or in areas where skin folds, like the elbows or behind the knees.
While in some individuals, eczema can present as small patches of dry skin, others with more serious forms of the condition may experience widespread pain and inflammation of the skin all over the body.
On lighter skin, inflammation from eczema can present as reddish in tone, and on darker skin, ‘patches’ of inflammation may appear as brown, purple or grey. As a result, many patients with darker skin tones may find the condition difficult to see – which can result in frustration and delays in obtaining a medical diagnosis.
While some aspects are common across each type – like dry, scaly skin, discolouration and itchiness, which may be intense – there are actually 7 different kinds of eczema.
Types of Eczema
While all types of eczema can cause distress, some may present more serious issues than others if left untreated, or if treated improperly. Scratching or otherwise interfering with eczema may cause infection or other complications, so it is important to seek medical advice if the condition persists or worsens.







Causes of Eczema
Some eczema is caused by allergies, or contact with chemicals and certain metals, but there may be other causes – for example, genetic predisposition; problems with the immune system function; environmental factors; infections; skin dryness; or stress.
Research has shown that patients may have a genetic tendency to suffer from the ‘atopic triad,’ these allergic conditions are allergic rhinitis (hayfever), asthma and atopic dermatitis (eczema). They often run together and in families.
Different types of of eczema may have specific causes.
Whatever your needs, you can rest assured that Derma will provide the very best care for your skin, with access to the latest research and treatments.
Treatment of Eczema at Derma
Whilst there is no cure for eczema, in many cases it can be controlled using moisturisers and intermittent use of topical steroids. If symptoms recur and remain uncomfortable, patients should consult a dermatology expert for treatment.
What to Expect
Your appointment to assess and treat eczema will begin with a skin check and medical history, followed by a discussion on the recommended treatment options.
Your dermatologist will explain the potential limitations and side-effects of each treatment.
Due to the specialised nature of dermatology, and our significant experience in treating eczema, our experts are likely to be able to prescribe treatments more effective than those prescribed by GPs.
These specialist dermatological treatments can more quickly and effectively control and manage eczema, eliminating all the symptoms so that there is no more discomfort. In many cases, this level of comfort can then be maintained.
For more delicate areas, or for prolonged treatment, Derma is able to offer alternatives to steroid treatments – such as light treatment (also known as phototherapy); and for more severe eczema cases, it may be possible to prescribe tablets that help to better regulate the immune system.
For more information, or to book an appointment with Derma, please call the clinic or contact us via email here.
Frequently Asked Questions
Eczema is not contagious and can’t be caught from someone or something else. Eczema is a complex skin condition that is caused by a combination of genetic and environmental factors. Eczema is very common and whilst it commonly occurs in childhood, it can occur at any age at any site of the body.
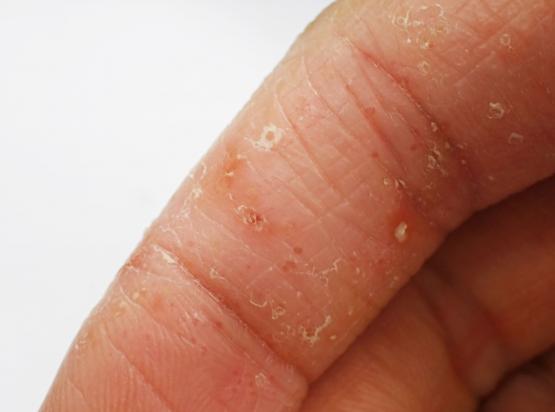
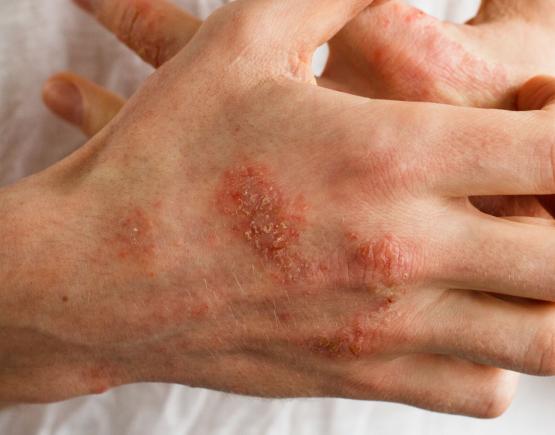
Hand eczema occurs when the skin is irritated and it results in red, sore and often split skin that can be very itchy and uncomfortable. Trying to minimise contact with substances that irritate the skin can help but this is not always possible as even water can dry out the skin. It occurs as a result of a combination of both genetic and environmental factors. Treatment is aimed at protecting the skin and reducing the inflammation.
Stress will not cause eczema but it can certainly make it worse. During periods of stress, we release more cortisol which is a stress hormone. Cortisol can lead to inflammation which will aggravate the skin.
Send an Enquiry